
Breathe Right please sponsor me! I recommend everyone try Breathe Right strips. A pack of 30 is $9 and they’ll even send you the first pack for free.
https://www.breatheright.com/samples-sign-up
New EA cause – get everyone to try nasal strips. The positive impact of better breathing at night for the low price of $0.30 is an insane cost / benefit. Even if they do nothing for you, they’ll come in handy when you catch a cold.
How I figured out I have sleep apnea
I was always super tired in the morning and about every two weeks I’d have a situation where I’d wake up gasping for air. I never really paid attention to it, because I figured that this was normal.
Thanks to a Facebook advertisement, I decided to take the Lofta sleep test, which revealed that I have sleep apnea with an AHI (how many times you stop breathing per hour) of 18 and RDI (how many times your breathing is obstructed per hour) of 26. This is classified as moderate.
I followed up with an ENT to take a look at my throat. Viewed through an endoscope, it was obvious that my tongue was too far back, close to obstructing my airway.
I figured that while CPAP is a decent solution, it’d be a good idea to test some less annoying ways of fixing my sleep apnea. The masks are rizzless, see below
A quick aside though – CPAP is the gold standard therapy for sleep apnea. Don’t use this article as an excuse to not treat your sleep apnea!
I’ve managed to get down to an AHI of 8 thanks to the didgeridoo. More on that later!
Sleep apnea
Sleep apnea is where your breathing stops and then restarts during sleep. This can be either due to airway collapse or because your brain forgets to send a signal to your body to breathe. Your brain forgetting to breathe is pretty rare and called central sleep apnea. Most treatments here will have no effect on central sleep apnea — if you do have it you should go on a CPAP since you’re literally forgetting to breathe.
Obstructive sleep apnea, where your airway collapses, is generally because your airway muscles relax during sleep. The main forms of obstruction can be split into four anatomical sources: the soft palate, the oropharynx, the tongue, and the epiglottis. This is the VOTE classification — sleep apnea can usually be decomposed into obstruction at one or more of these four sites.
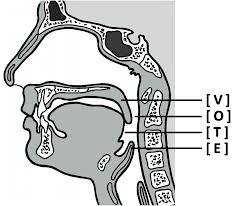
Figuring out which site is the problem is typically done one of two ways: educated guessing (like I did), or — if you want to be scientific about it — a drug-induced sleep endoscopy, or DISE. DISE involves putting the patient under sedation, then using an endoscope to see which structures are collapsing.
It’s unfortunately expensive, but worth it if you can’t figure out which part of your airway is giving you trouble and want to try out non-CPAP solutions, since each obstruction site points to different interventions.
Do you have sleep apnea?
If you’re wondering whether you need to get a sleep test — you absolutely should. They’re very affordable and a one night, take home test will tell you whether you’re getting good sleep.
- Any amount of snoring means you are far more likely to have sleep apnea, which I don’t think people realize. If you snore, even quietly, it’s definitely worth checking yourself for sleep apnea.
- Jutting your jaw out or grinding your teeth during sleep means your body is trying to get more air into your lungs — also a warning sign. If someone wakes up earlier than you, you can ask them to check for these signs.
- Finally, an underrated sign is waking up to pee in the middle of the night. When your airway collapses, you keep trying to breathe against it, which creates a vacuum in your chest that stretches your heart. Your heart panics that it’s overloaded with fluid and signals your kidneys to drain the tank — so you wake up needing to pee. If you’re waking up to pee every night, it’s absolutely worth getting a sleep test to eliminate that as an issue.
I can say from personal experience that getting sleep apnea treated is definitely worth it.
Sleep apnea is bad
Sleep apnea as an illness doesn’t kill immediately. It’s very unlikely that you’ll simply choke to death in the middle of the night. The human body is good at staying alive. What happens instead is that you’ll wake up a bit, regain muscle tension, catch your breath, and then go back to sleep. Sounds innocent, but there are a ton of downstream problems.
- You get woken up — this fragments your sleep and reduces your time spent in deep & REM sleep. The result is that you feel like absolute crap. You may spend 8 hours in bed, but it’ll never be restful.
- The way you get woken up is your body panicking that it doesn’t have enough air. You get shocked into wakefulness with a spike of cortisol and adrenalin. Your blood pressure and heart rate spikes.
- High blood pressure from sleep apnea brings with it a ton of issues, more than I’d care to list here — but one particular issue worth mentioning is kidney disease. Your kidneys slowly get destroyed by the blood pressure spikes.
- The constant heart rate and blood pressure spikes bring heart disease.
Note that often you don’t remember all of these micro-wakeups. I was not breathing 18 times per hour. I only remembered waking up maybe two or three times per night.
Frankly — the worst part for me was the mental effect of sleep apnea. I felt like a complete zombie. I was yawning the entire day, I needed 3 cups of strong coffee to get my day started, I had a terrible memory. I couldn’t really think straight for long periods of time, my brain would slide around off of topics. Obviously — if you’re not sleeping well, you don’t function normally, but the issue is that it feels normal to you. I used to think that I slept fine (hah) and that feeling completely exhausted at all times was pretty normal. We’re all chained to our own reality, so it’s hard to judge whether you’re actually constantly tired compared to the human norm. It wasn’t until I started resolving the sleep apnea that I actually realized how cooked I was.
A question I hear often is — why is sleep apnea so common now? Unfortunately, the modern diet of soft foods means that our jaws are drastically underdeveloped compared to the jaws of people living in the pre-Industrial era. This means there’s less room for the tongue in the mouth, leading to the tongue falling back into the throat. The modern diet and predilection for cleanliness also mean allergies are far more common — leading to nasal breathing issues. Throat collapse can be caused by many factors, but the most common are obesity and age. Obesity is a modern problem, and can also traced back to the Western diet.
Measurement
In order to properly measure the impact of interventions, I’d have to measure my sleep somehow. There aren’t a lot of options unfortunately.
Oura Ring – it measures sleep quality in a general sense, not specifically sleep apnea. It does have a blood oxygen measurement feature, but it’s not very sensitive. I decided to buy one mostly on the theory that improved sleep apnea would likely correlate with better sleep in general.

Wellue O2 ring – I’m not sure why continuous pulse oximeters are so hard to find (glares at FDA?), but this one does the job. It measures my sleep apnea decently well. The only issues I have with it is that 1. if I toss and turn too much I get bad readings 2. The rubber ring has started to wear out, which I counteract by putting on progressively larger fingers.

Lofta sleep test – This is the test I used to get a formal diagnosis. It’s usually $189 for the test. Lofta ships you a pulse oximeter which is connected to a single EKG lead that you attach to your chest. You connect it via an app, measure for one night, then discard the hardware (!!!). Someone please hack this thing so it’s not such a horrible waste. You then get a call from a doctor who discusses the test results with you and tries to sell you a CPAP from Lofta.
Sunrise sleep test – I haven’t tried this but it looks really cool. It measures sleep apnea with a sensor placed on your chin. The idea is that your jaw moves forward to counteract a collapsed airway, so by measuring jaw movement you can determine respiratory effort.

Medical treatments
I always recommend people start with a simple sleep test, because it’s difficult to know how aggressive to be with treatment until you know how bad the problem is. If you have severe sleep apnea, you should definitely get on a CPAP as soon as possible, before even considering other therapies.
The CPAP is unfortunately the gold standard for sleep apnea therapy. The truth is that it’ll resolve sleep apnea entirely when you use it — the problem is most people absolutely hate using it. The adherence rate on the CPAP is around 50% of people who try using it. This is crazy, because it’s a life saving device that makes you feel like a real person again. The reason why compliance is so poor is because you need to wear a mask every night that pumps air into you to ensure you can breathe. Some people also say that while it fixes their sleep apnea, it also ruins their sleep because of discomfort.
I think a lot of the adherence issues could be resolved by understanding that beginning with a CPAP is only the beginning of a longer journey. There’s quite a bit of work that goes into ensuring the CPAP works for you — there are a lot of settings to tune and different masks to try. This requires a bit of agency, which is disheartening to hear after the CPAP is heralded as an end to sleep apnea. On the bright side, for those who stick with it, it is very worth it. Many CPAP users resolve their sleep apnea and are happy with their machines.
The iNAP is a CPAP alternative. It’s basically the suction tube they use at the dentist’s office to suck the saliva out of your throat, but you put it above the tongue instead to suction it to the front of your mouth. This pulls your tongue and associated tissues out of your throat and makes more room for air to pass. It’s a funny solution, but it’s very helpful when your tongue doesn’t fit with your jaw size. See image below.
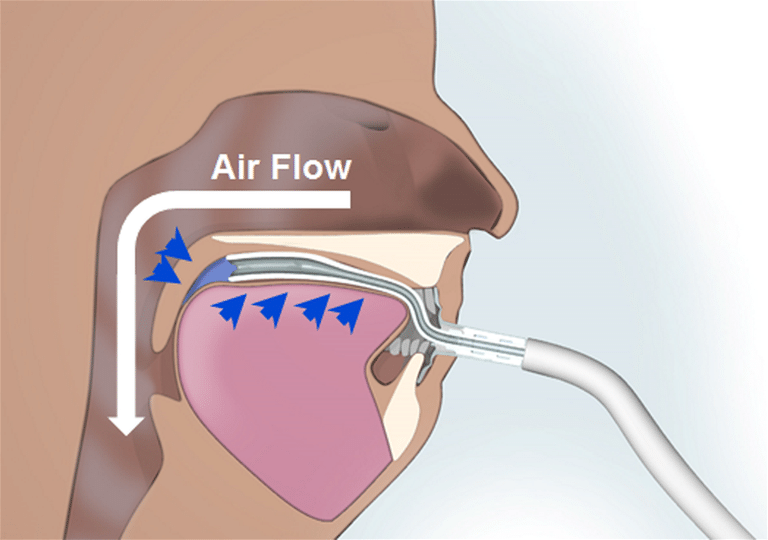
I’ve started iNAP therapy — I diagnosed myself with primarily tongue based sleep apnea off of an educated guess. I’ve been having great results! I find it reasonably pleasant to sleep with since it’s quiet. The only annoying bit is cleaning the saliva from the tubing every morning. I highly recommend it if you have tongue based sleep apnea. I haven’t done a sleep test confirming whether it dropped my AHI, but I’m dead certain it’s improved things.
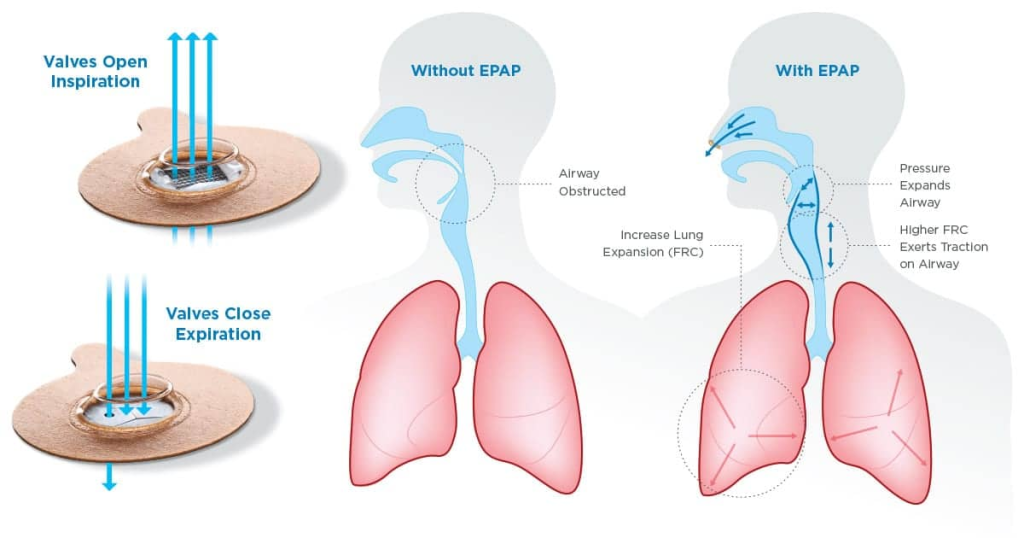
Bongo RX is a nasal-only insert that takes advantage of creating back pressure on your exhalation. When you breathe out, there’s reduced pressure on your throat, which allows it to collapse. If you maintain some small amount of pressure, it should prevent the collapse. Diagram & image below.

Note: I’ll use the word “shock” to describe what the next few devices are doing, but it’s less of an electrocution and more of a gentle pulse. Nobody’s looking like this —

Inspire is a bit hardcore for my tastes, but it does appear to be super helpful for people. It involves surgically implanting the equivalent of a pacemaker that then shocks your esophageal muscles every time you take a breath. This ensures that your airway has the same level of openness as it does when you’re awake and your muscles are tense. Downside is that it requires surgery.
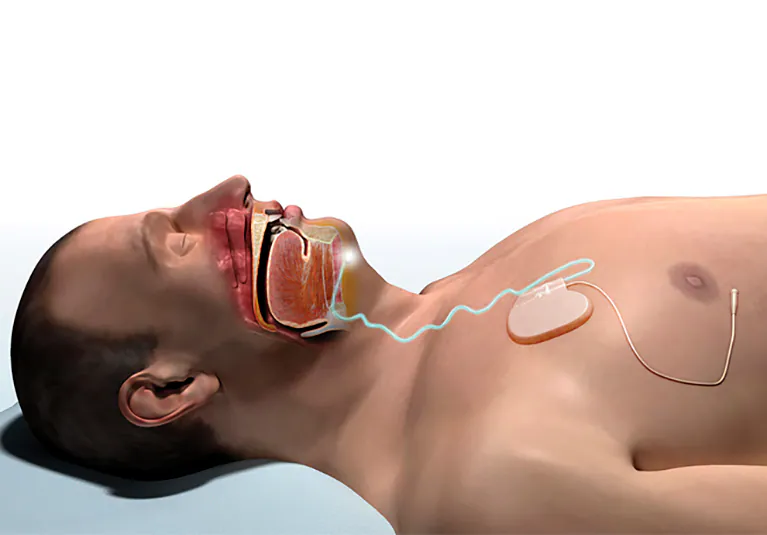
Zeus is basically Inspire but without the surgical implantation step. You attach it to the bottom of your chin and it shocks the tongue & jaw muscles through the skin.

ExciteOSA is a fascinating product — exercise in a device! If you don’t have the executive function to stick with the tongue exercises, you can try using this instead. You put the device in your mouth and it shocks your muscles to exercise them. You use it for 20 minutes per day for 6 weeks.

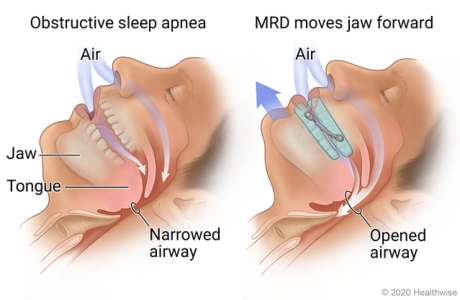
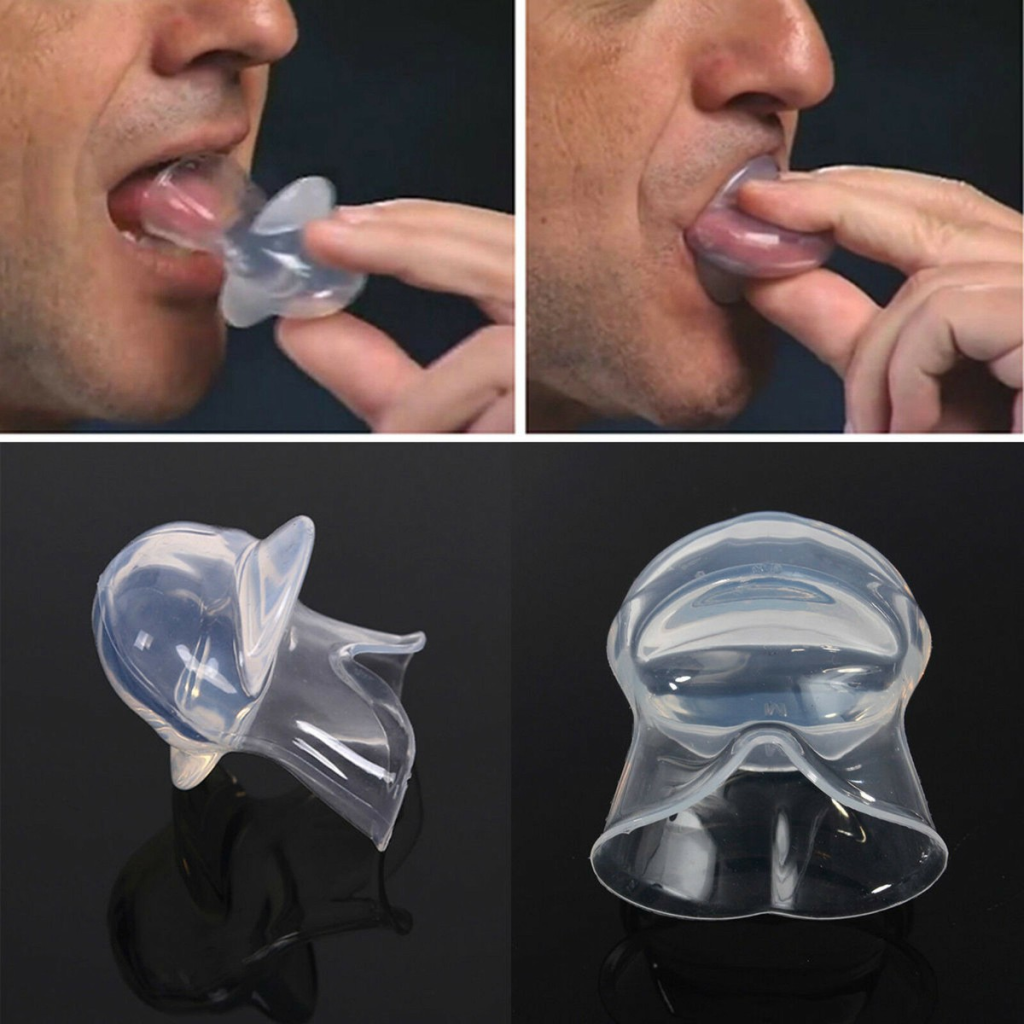
Oral appliances are generally anything that manipulates your mouth physically to prevent sleep apnea. They fall into two main categories, mandibular advancement devices and tongue retention devices. Mandibular advancement devices shove your jaw forward, which should open your esophagus more. Tongue retention devices grip your tongue and thus prevent it from falling back and choking you. I can’t use the jaw advancer since I have TMJ, but you should feel free to try! Tongue retention devices are notoriously uncomfortable since they’re usually grabbing your tongue.
Surgery is an option, but I don’t know much about it. I’d be careful if I were you.
Lifestyle interventions (listed from least woo to most)
Sleep position – this is by far the best effort to results item on this list. If you currently sleep on your back, try sleeping on your side. There are countless ways to achieve this, so I won’t bother listing them all, but suffice to say they work by mechanically forcing you to sleep on your side. (Un?)Fortunately for me, I’m a lifelong side sleeper. Interestingly though, the O2 ring and Oura helped me discover a position issue during sleep. I usually sleep hugging a pillow, but for a short period during a move I slept without one. My sleep and oxygen scores were significantly worse! It turns out that hugging the pillow were helping my breathing by preventing me from flopping onto my stomach. The takeaway for you should be to experiment with various position interventions.
I started with the wedge pillow, since it was the easiest of the interventions. Unfortunately, it was a total failure, with my sleep apnea appearing to only get worse. You can also try tilting your bed.
Nasal breathing! Mouth taping appears to help some people by preventing you from breathing through your mouth. The theory goes that you can reduce snoring, improve mouth position, and take advantage of the benefits of breathing through your nose.
Nasal strips, as previously mentioned, can be a lifesaver. I don’t even have nasal based sleep apnea but just having an open nose is super helpful in having better sleep quality.
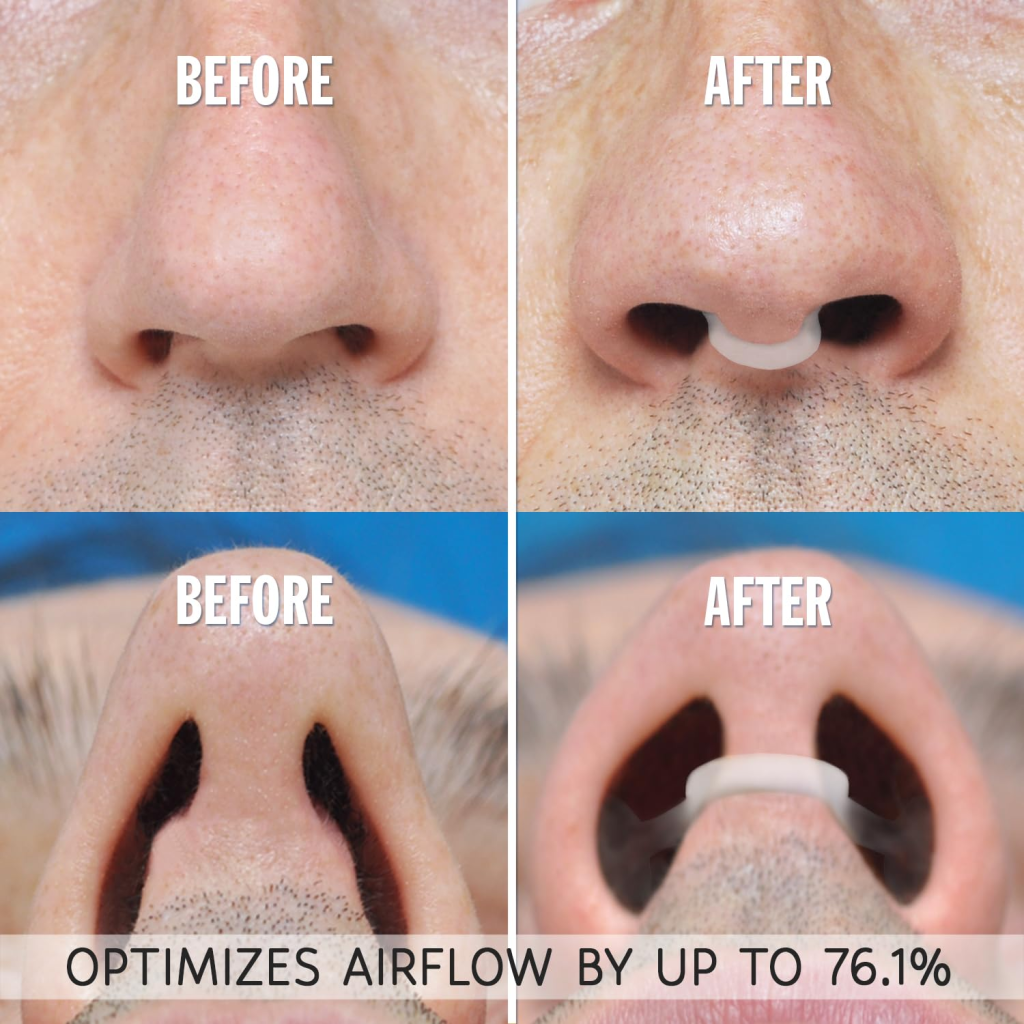
Nasal dilators are an alternative to nasal strips where rather than pulling open your nose through an adhesive on the outside, they push it open from the inside with a plastic bit. I tried them and found that they feel exactly like having a piece of plastic in your nose. My friend, however, prefers them to nasal strips — he says they’re easier on the nose skin.
Weight loss can help a LOT with sleep apnea. If you have less fat in your airway, you’ll have less to collapse. Sleep apnea tends to cause weight gain, so treating sleep apnea can actually help you lose weight as well. I’m at a normal weight, so not much relevant here for me.
Exercise can help a lot, but I already exercise. If you don’t, you really should, and not just because of the sleep apnea.
Vik Veers says that only 6% of patients exclusively have a tongue issue. On hearing that, I thought I’d try Flonase to have a bit easier time breathing through my nose, hoping that it’d have an effect on my sleep apnea. Unfortunately, while I did subjectively feel that it improved my sleep quality, it didn’t affect my Oura or O2 scores. You can use Flonase continuously for up to 6 months, which should cover you for allergy season. Note that you can use it longer — but you should check with a doctor if you want to try that.
Azelastine is another nasal spray specifically for allergies. It’s an antihistamine that you can spray directly into your nose, which means it works significantly better for opening up nasal passages. Do note that there’s a specific spraying technique you should use to avoid getting it into your throat since it tastes terrible. I use azelastine during peak allergy season. It apparently may help protect against COVID too? I suggest avoiding alcohol when using azelastine, I’ve noticed it decreases my tolerance significantly.
Afrin deserves a mention since it should not be used for sleep apnea treatment. It’s a powerful decongestant, but you can’t use it for longer than three days. If used longer, you end up with rebound congestion that is worse than when you started using the medication. I personally use it exclusively when I’m sick and I can’t breathe through my nose at all. Otherwise, I recommend staying away entirely.
There’s some evidence that mouth exercises can help with sleep apnea. Here are some links to a research paper and a Reddit post about various exercise techniques. Since my apnea is mostly tongue related I tried doing this set from Vik Veers. I didn’t seen much in terms of effects. If you want exercises in a nice app format, check out Airway Gym.
Have you wanted to learn an instrument? No? Me neither, but here we are. There’s some (sketchy) evidence that playing specifically either a double reed instrument, which is the oboe, or a didgeridoo can be protective against sleep apnea. The suspected mechanism in the didgeridoo appears to be the circular breathing, which doesn’t make sense because many woodwind instruments require circular breathing. The oboe may be useful since you need to generate high pressure in the mouth and also move your tongue to play music. In any case, it’s worth trying, but don’t hold your breath (hah).
I’ve been playing the didgeridoo now for 3 months — I’ll be taking a follow up sleep apnea test soon. Will report back with results.

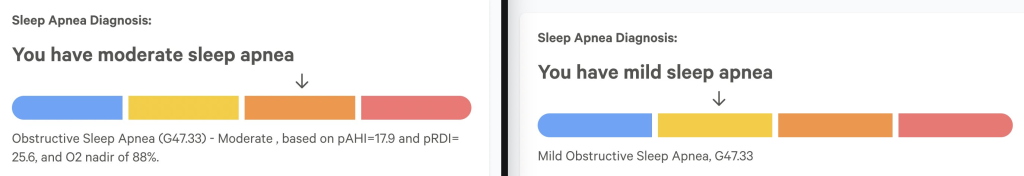
Update: I’ve been playing the didgeridoo for about half a year now. Great news, it seems to have worked! Results below. I play 25 minutes per day, 6 days per week. I recommend getting started with this video and a PVC pipe didgeridoo.
Myofunctional therapy is a method by which you train your tongue and mouth muscles in order to have them collapse less during sleep. There’s some good evidence that it provides a mild benefit, but obviously it’s more expensive than a PVC pipe didgeridoo — because of that I have no personal experience with it. I’d recommend trying it if you can’t stomach 25 minutes of didgeridoo per day or if your spouse can’t.
Buteyko breathing is a technique by which you work to increase your CO2 tolerance. In theory this should help with sleep apnea symptoms since you’ll have a lower reaction to holding your breath (which in this case is choking on your own throat). Buteyko does seem to work for freediving, so maybe it works for sleep apnea, someone please try and report back.
Mewing is a practice invented by John Mew to expand the palate in order to increase jaw size. It’s unclear as to whether it works, and if it does work, it’s unclear if it would resolve sleep apnea. Mewing is where you suction the tongue to the roof of the mouth, thereby expanding the upper jaw. The theoretical mechanism by which it could address sleep apnea would be — larger jaw -> more room for tongue in jaw -> less tongue collapse. It probably wouldn’t address issues with throat collapse.
People on Reddit say Wim Hof breathing helped, but frankly I’m not certain by what mechanism it would help with sleep apnea. Let me know if it worked for you?
Conclusion
There really aren’t any silver bullet solutions here, unfortunately. On the bright side, if you’re willing to accept some tradeoffs — sleep apnea is a reasonably tractable problem. If in doubt, get yourself a sleep test.